Behavioral Health Revenue Cycle Management Requires Better Claims Communication
Behavioral health leaders often assume their revenue challenges come down to billing performance:
“Our billing team isn’t following up enough.”
“We need better denial management.”
“A/R is creeping up—we need more staff.”
Those assumptions feel logical. They’re also usually wrong.
What most practices actually have is a claims communication problem—and until that’s addressed, no amount of staffing, outsourcing, or software switching will consistently fix revenue.
The Illusion of Billing Issues
On the surface, the symptoms point to billing:
- Denials increasing
- Claims sitting unresolved
- Cash flow lagging
So the response becomes:
- Add more follow-up
- Send more emails
- Hire more billers
But step inside the workflow, and a different pattern emerges.
- A denial comes in.
- Someone interprets it.
- A message gets sent.
- The practice is unsure what to do.
- Time passes.
- The claim stalls.
The issue isn’t effort—it’s translation.
The Real Bottleneck: Fragmented Communication
In most systems today, the claims lifecycle looks like this:
- Claim is submitted
- Denial or issue is returned
- A ticket is created
- A team member reviews it
- A message is sent to the practice
- The practice tries to interpret and respond
At each step, context is lost.
A denial code might say one thing—but the actual issue is something else entirely:
- A COB denial that’s really an eligibility sequencing issue
- An authorization denial that should have been caught pre-submission
- A request to “verify insurance” with no explanation of why
So the practice delays, asks questions, or takes the wrong action.
Meanwhile, the claim sits.
Claims don’t stall because they’re complex.
They stall because no one translates them into clear, actionable steps.
The Hidden Cost of Chat and Tickets
Most organizations rely on some combination of:
- Slack or Teams
- Ticketing systems
These tools create the appearance of activity—but they introduce significant inefficiencies:
- Multiple back-and-forth messages per claim
- Repeated explanations of the same issue
- Offshore teams calling payers without full context
- Senior staff acting as translators instead of operators
The result:
- Higher cost per claim
- Slower resolution times
- Increased write-offs
- Frustration across teams
This is where revenue quietly leaks—not from lack of effort, but from lack of structure.
What High-Performance Claims Systems Actually Do
High-performing revenue cycle operations don’t rely on more communication.
They rely on better-structured communication.
That means:
- Every claim has a clear status
- Every issue has a defined root cause
- Every action is explicitly guided
- Every team member sees the same information
Instead of asking:
“What should we do with this claim?”
The system answers:
“Here’s the issue. Here’s why it happened. Here’s the next step.”
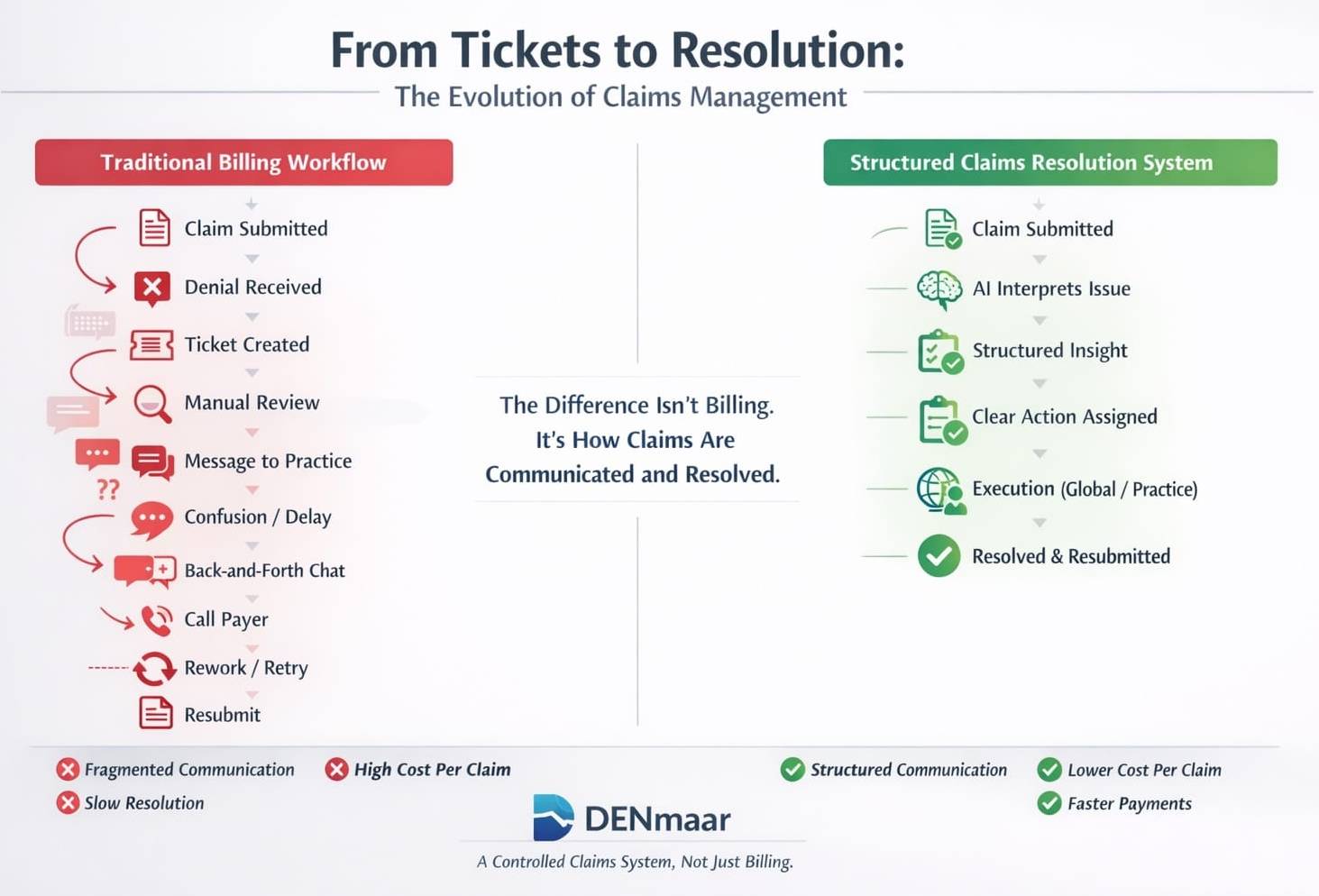
From Tickets to Resolution Systems
Consider the difference:
Traditional Ticket
“Please verify insurance.”
Structured Claims Communication
“Secondary insurance detected. Primary payer likely changed.
Action: Contact patient to confirm active plan and update payer sequence before resubmission.”
One creates confusion.
The other drives resolution.
This shift—from vague tickets to structured, claim-specific guidance—is where performance changes.
Where AI Actually Fits in Behavioral Health Billing
There’s a lot of noise around AI in healthcare right now. Most of it misses the point.
AI is not valuable because it replaces people.
It’s valuable because it standardizes interpretation and accelerates decision-making.
In the claims lifecycle, that means:
- Translating denial codes into real-world causes
- Identifying patterns across payer behavior
- Recommending next steps based on historical outcomes
- Reducing unnecessary payer calls
AI becomes the interpreter and guide, not the operator.
Learn how this works in AI behavioral health billing and clean claims systems.
Why This Breaks at Scale
At low volume, teams can “manage through it.”
At higher volume, the cracks widen:
- 500 claims/month → manageable
- 5,000+ claims/month → breakdown
More claims mean:
- More variability
- More payer nuance
- More communication points
Without a structured system, complexity compounds—and revenue suffers.
What works for a small practice doesn’t scale to a growing group.
The Shift: From Billing to Controlled Claims Systems
The most important shift isn’t hiring more staff or switching vendors.
It’s moving from:
Reactive billing workflows
To:
Controlled claims systems with embedded communication logic
At DENmaar, that’s been the focus:
Not just submitting claims—but controlling the entire lifecycle:
From scheduling
To documentation
To claim generation
To post-submission resolution
With structured communication and embedded intelligence at every step.
This includes:
- Behavioral health EHR software
- Mental health billing services
- Claims hygiene workflows
- AI progress notes for behavioral health
- AI front door patient intake systems
Final Thought
If your team is spending more time explaining claims than resolving them,
you don’t have a staffing issue.
You have a system issue.
And fixing that changes everything:
- Faster payments
- Lower cost per claim
- Less friction across teams
- Stronger, more predictable revenue
That’s where the real leverage is.